TABLE OF CONTENTS
- INTRODUCTION
- “…OFFERRING HELP…”
- “IT DEPENDS ON THE CASE…”: THE PERSONAL COST.
- “THE PANDEMIC, A LESSON FOR ALL OF US.”
- “THE TOUGHEST TIMES.”
- CONCLUSIONS
- BIBLIOGRAPHY
- NOTES
INTRODUCTION
2020 was the year when everything changed. A deadly virus spread all over the world leaving numerous victims behind. COVID-19 was declared by the World Health Organization as a “public health emergency” in January 2020. 1 This new pandemic has similarities with previous ones but it also has unique stressors due to the high rate of asymptomatic contraction of the virus. 2 In March 2020, SARS-COV-2 was officially declared a pandemic as it has already infected more than 200 countries worldwide. 3 It affected not only those who were infected but also their families. But mostly it affected the front line health workers who gave a tremendous fight with the virus and are still fighting it. Someone could say it altered their personalities; it changed who they are, not only as employees but also as human beings.
This is what I am trying to explore through my research: the psychological effects of COVID-19 on the front-line health workers. Their personalities and views were definitely transformed by the pandemic, but how and why? Did their work-position contributed to them being afflicted or not? I interviewed four health workers living and working in a small town in the region of Aitoloakarnania, located in Western Greece. Two of the interviewees are my parents: my father (Theodoros) is an Emergency Μedical Τechnician (EMT) and my mother (Alexia) works for the Mobile Teams of the National Public Health Organization. The other narrators both work as Emergency Medical Τechnicians and are married to each other, Konstantinos and Dimitra. Konstantinos got infected by the virus so it was for me really fascinating to hear his experience. As a daughter of two front-line health workers, I have a personal stake in our current situation, but I am especially interested in the psychological and emotional toll of COVID-19 on those who work in healthcare, not only during their stints at the workplace, but also when those people come home after a long shift. What impact has this struggle on their inner self and their private lives? Are there any similarities between the psychological impact of the virus abroad and Greece, especially in a smaller town like the one my narrators work at? Has it become an easy process for them through time? Can we say that Coronavirus has become a common healthcare problem by now? Or was it a life-changing event at the end? As stated before, my interviewees work in a small town somewhere in Western Greece, which means that the relationship between patients and health workers is more intimate than in big cities.
“OFFERRING HELP…”
In Greece, COVID-19 cases increased slowly, at the beginning, back in the spring of 2020. The virus infection rates were not equally distributed. The National Health System, the government, and the whole society were unprepared for what came next. The real “boom” came after the end of the summer of 2020. COVID-19 cases kept increasing rapidly and the beds in Intensive Care Units weren’t enough. There was a big crisis on its way. Official data indicate that Greece turned around the disease with minimum casualties until September 2020. However the 2nd wave of Coronavirus afflicted the country and swarms of people died every day. By late July of 2021, 458.000 people have been infected and approximately 13.000 of them have died. 4
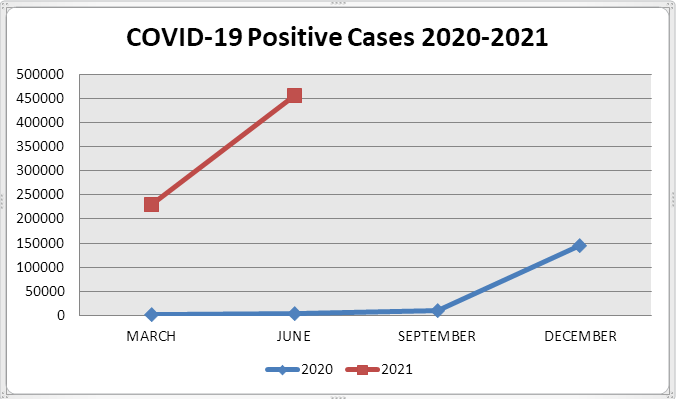
The medical staff was physically exhausted and emotionally drained. A study about the psychological effects of COVID-19 on health workers in China shows that having a daily work so high at-risk puts your physical and mental health at stake. 5 It is a very serious risk, especially because many of those in treatment are asymptomatic, which makes the transmission of the virus undetectable. My town, in particular, has been put in the “high risk” category only twice. Despite that people kept dying and friends and family members kept contracting the virus. The local hospital was by all accounts unprepared for the pandemic. Personnel shortage and lack of equipment thampered its ability to treat patients. In June, 37 out of 41 COVID-19 patients that were transported to the hospital died. Everyone knew, and everybody highlighted the negligence displayed by the hospital administration, but nothing changed the fact that those people could have been saved. 6 Given these facts, how can anyone feel safe in that hospital, either as a patient or as an employee? Someone could say that not knowing who is going to be next made our daily lives, a living nightmare, like disasters we read in history books.
It is time to provide more details about my interviewees’ occupations. Theodoros, Konstantinos and Dimitra work in EMT. Theodoros has serviced as an Emergency Medical Technician for 31 years, Konstantinos has been working for 22 and Dimitra for 15 years respectively. They are paramedics, responsible for transporting patients to the hospital. During the transportation, they have to give first aid care to those people in need and are obliged to wear a special suit in order to protect themselves. My mother on the other hand, works in a mobile unit and goes every day to different places conducting rapid tests in order to find people that are positive and inform them about what to do next. She was hired not long before the second wave of the virus hits the city. The authorities needed more helping hands to deal with the massive rapid testing process. My mother and her colleagues were firstly hired on a three month contract but the increasing number of casualties, made their indentures renewed every now and then. Sometimes she had to stay at work extra hours depending on the number of people that came to do the test. In similar fashion EMT workers regularly have to transport patients to other hospitals in Greece, so they also have to work overtime. Nevertheless, unlike other studies which revealed that many front-line health workers suffered from burn-out, my interviewees never mentioned that. It made me think that it might be due to their type of work. They are paramedics, so they never had to work double shifts when the positivity rate was high. More importantly they do not work inside the hospital. Nurses or doctors on the other hand had to work under extremely exhausting circumstances. 7
Now it is important to underline that those people bear a great responsibility to all of us. They are those who will treat us before we get to the hospital and will keep us alive until we get there, or they will advise us on what to do next. Among medical professionals, they are the ones closer to the populace. Sometimes it is an overwhelming experience but all my informers said they wouldn’t change their jobs. The fulfillment they feel by offering help and comfort to those who are afraid is what made them choose this job in the first place. As Dimitra said: “Being able to offer my help to someone who needs it is the best feeling I could get. I deal with patients before doctors, thus I have to deliver them alive and in the best possible shape. After a day that you possibly have saved a life, nothing else matters”. During their years’ work experience they have learned to be detached from the patients, and not bring their fears, anxiety, and frustration into their home. They all said that at first, handling the pandemic was really difficult, but having already dealt with the worst accidents and diseases toughened them up. But in the midst of a deadly pandemic like this one, how do they deal with the fact that the next patient may be their friend, their co-worker, or even a family member? They all said that the fact that this town is small, and everybody pretty much knows each other makes it more difficult than it would have been if they worked in a larger city. Konstantinos said that “of course the responsibility is the same to all civilians, you may be affected, but emotionally, transporting with the ambulance a stranger is not the same as transporting someone you know and love”. In the second case, you cannot maintain distance.

What about the National Health System? Did it support local hospitals or resources weren’t enough and they prioritized the larger hospitals? Moreover, was the training enough and well-explained? The EMT workers that I interviewed responded that they didn’t lack of COVID protection supplies (i.e. masks, suits, gloves, etc.) or special training. Theodoros insisted: “We had specific seminars on how to protect ourselves from COVID, how to put the protective suit the right way…and we may have a lack of medical supplies but not too often. It wasn’t on purpose though; the whole country was in shortage of medical supplies, I do not feel that we were left out.” These assertions contradict the data and the sources cited before that mentioned the lack of employees and equipment. Alexia said however that she was provided training from colleagues with more experience, not from an expert. But she never felt that she had no one to turn to for questions or guidance. She remembers though certain periods of time, when they had no rapid test supplies for 10 days in a row. The problems came back with the winter snowfall in Athens, when the highwayss were closed. Thus the molecular tests from my town never got to the lab in Athens. For almost three days all those people that were subjected to molecular tests had to stay in quarantine either way until they repeated the test. “But it wasn’t actually anyone’s fault, no one can predict the weather, but I think there should be a certain protocol in such cases in order to avoid this mess.”
“IT DEPENDS ON THE CASE…”: THE PERSONAL COST
Given their occupation, it is important to investigate how those people feel, what their emotions are and how they react to the pandemic. Alexia started working in September 2020. It was not long before the second wave of COVID-19 hit Greece, with detrimental consequences. She had to learn the task at hand quickly from other colleagues and soon she felt ready to begin. But then scientists traced new mutations of the virus and that meant… new training was required. “There was a time where we received, different information from the Health Ministry about the virus, about the rapid tests, about the practical-technological stuff every week.” This is a situation that did not only happen in Greece. According to a study by the US National Library of Medicine, continuous changes regarding personal protective equipment made health workers unsure about their work-safety. 8 9 As Alexia was about to start working, my home town started to register dangerous levels of infections the period before Christmas. A question that truly worried me was about her first Coronavirus-positive patient. She said that she was a middle-aged lady that came for a rapid test and found out she had contracted the virus. My mother was nervous, she was afraid of the patient’s reaction. But surprisingly, the lady was so calm and she only asked what she should do next. It was then that she realized that she was closer to COVID-19 than most of the people and that the disease was real and dangerous.

After that, I could not but ask how it feels to announce to someone that he/she is positive. She responded that she is “immune” to that now. She still feels sorry and will be compassionate towards the infected, but it does not affect her that much anymore. She pointed out that society has grown more resilient to such news; people handle the news better than they did one year ago. All interviewed EMT workers agreed that initially it was a shock. They still remember the curiosity and the fear of an “unknown” virus and what it can do. What about the work itself, had COVID changed the way they feel, perform their duties, or react to everyday occurrences? Well, all four informers mentioned that they feel they have a debt to the society; they have to be prepared, resilient, ready to “save lives” or just be there for those who can’t cope with the situation. But mostly they realized they owe to themselves and their families to stay mentally and physically healthy. Dimitra said: “…we can’t let it drag us down, because then it will consume us…” and by that she means that what happens at work stays there. When they take off their medical scrubs they leave their job behind. From the time their shift is over, they are no longer an EMT or a National Health Organization worker; they are parents, husbands and wives, brothers and sisters. They learnt that by experience. Their families could be destroyed if they brought their anxiety to the family table, their nerves and even the pain of those they lost that day, the EMT staff said. Theodoros observed that “…only in rare cases I will discuss with my wife something that happened at work that day. It has to be something that shocked me and I can’t let it go.”
Given EMT staff’s experience at work, I wondered whether COVID patients are included in the “bad cases” category. Unanimously my interviewees said that they have seen the worst accidents someone can have, they had to save someone that had so many wounds that could be already dead, they have seen young people dead or having suffered terrible accidents, and people in tremendous pain… COVID-19 patients have a pretty good chance they will survive and come back home to their families, while a car accident victim could have zero chance. In fact, he or she could be dead even before the ambulance gets there. In this regard, the bouts of the pandemic definitely affect them but not as much as other cases do. Konstantinos mentioned that “Well, every case is different, some make our hearts heavy, some keep us up all night wondering what happened to that person, some make us happy and some don’t affect us at all. It depends on the case, the personality and the relationship with the patient.” Fear will be always there, they cannot avoid it, either in the past or now. To that point, I asked if the fact they know more than the average person about the virus makes them treat the subject more prudently. The response surprised me; they all agreed that the fact they know more than us is not always a privilege. They are not doctors, hence they do not know nearly enough, but they still are more informed which can lead them to fear the worst-case scenario over a mere fever. The same thing applies to COVID-19; the simplest sneeze or sore throat makes them anxious. They know more than us, but not enough in order not to panic. It is not their job to diagnose a patient, but when it comes to their family, they said that their head explodes with ominous possibilities over the simplest things. Knowing what may occur if someone contracts the virus makes them more vulnerable when hearing that some member of their family, a friend or a colleague tested positive. Lastly, and somewhat paradoxically, being that exposed to the virus makes you worry, but in the end, you kind of get used to it. You protect yourself in every way you can, you definitely are afraid of infecting your kin but life goes on and we have to keep living.
“THE PANDEMIC, A LESSON FOR ALL OF US.”
On that note, I persisted with questions focused on their emotions. All my sources acknowledged that the pandemic altered their profession and their emotions around it. Even before the virus, they had high tension duties, but now they have one more responsibility towards society and their relatives. As Konstantinos explained well: “Of course we changed, our work has changed. Before COVID-19 our worries were less and the danger of contracting the virus to our families definitely was not that high. Now one simple mistake, like not following the suit protocol could endanger my wife. Before the pandemic, there was barely any fear for anything. ” Theodoros on top of that added: “For 31 years I work in pre-hospital care and the virus made me realize that the anxiety of keeping the patient alive can be doubled if I suspect that I am the reason my family may get sick. We offer help but we fear too, maybe now not that much but we do. We can’t show it but it is there.” Now that this aspect was covered, I continued with a question that I was excited about… What will they keep from the exigency the whole country and the National Health System is experiencing. A very interesting response came from Alexia. She pointed out that after the Coronavirus emergency is over she will be left with thoughts about the rapid social changes, the evolution of Medicine and the numerous new fatal diseases that may occur. But she is also concerned about unprepared facilities, off-guard political leaders and the impassivity of modern societies. Theodoros noted: “I am worried about the future, about the world my kids and grandchildren will live. One pandemic shut down the whole world and we have barely recovered yet. Humanity walks in a very dangerous path.” He proposed that, first of all, ordinary people gain their compassion back and start caring about their fellowmen. All people have to be conscientious for everyone’s sake. But he also suggested that this mishap can become a lesson for everybody, especially the governments in order to be prepared in the future. From a totally different point of view, Dimitra sounded optimistic about the future. She stated that chaos may happen, but humanity can cope with and evolve after that. Some of them won’t forget the experience, but it seems that it will get buried in their minds and their hearts sooner or later.
As I mentioned before, I have a personal stake in these stories. All the interviewees are family, or like family to me. Along with them, during the pandemic, I experienced some emotions too. A brief example was the fear of coming anywhere near someone who had not a mask on. My mother always told me that COVID-19 is dangerous even to young ages like mine and that I should not risk infecting all my family. The fact that both my parents work in Health System occupations made it even more perilous. They could spread the virus to the hospital, affecting doctors, nurses and patients. I never felt threatened until some family members got sick. Two of my aunts have been tested Coronavirus-positive and were in a bad shape. I felt safe because my parents were careful, I was careful, thus I thought all the people around me knew. It was a shock having my aunt in the ICU for some days and hearing that she was in critical condition. Then friends (young-aged) contracted the virus and my parents were more exposed to the pandemic as the COVID-positive cases increased and some EMT staff contracted it. I felt like I was surrounded by the virus. That was when I decided I will return to Athens, where I am currently studying. I felt safer when I was alone in my flat, and in that way I could not put my relatives in danger. There was a period of time when I would take extreme measures before I got to go interact with people or even go to the grocery store. Now, over a year later I feel that humanity will survive this. I cannot lock myself in a glass jar and wait until it is “safe” again. As Dimitra said everything comes and goes.
“THE TOUGHEST TIMES”
Many people around us got infected. For me the first person who was really close to me, was Konstantinos. He was among the first ones who got infected in my hometown. It was also a huge shock for healthcare workers and for the EMT department. I was curious about his experience and the experience of others around him. Around the first trimester of 2020, he and Dimitra were in an EMT conference with other members of their trade union. They both were exposed to the same environment. They were in the same car coming back from the meeting and they live in the same house. Yet he got seriously diseased and she stayed healthy. Is virus “choosing” who to hit? The first thing he and his wife (Dimitra) pointed out was that it was the most difficult situation they have ever dealt with. It was so sudden they did not even know how to support each other. Konstantinos was in the ICU for approximately 15 days. Dimitra was quarantined all those days. She was not infected even though they both came in touch with the person who contracted the virus to Konstantinos. They were afraid for each other. Konstantinos mentioned: “I was so worried that I may have infected Dimitra and my mother that I could not rest even though my body was worn-down”. They contacted to each other sometimes, but he was unable to talk due to exhaustion. And, as Dimitra indicated, his inability to talk only made things worse for her. “Imagine being isolated in your house, alone, and your other half is fighting for his life and he is in such a bad shape that he can barely talk to you. I lost my sanity those days.” They both stated that they do not feel very comfortable talking about it, because it is something that they really try to forget. They only wished that nobody would ever experience something like that. But they agreed that it made them stronger, it brought them closer than ever. But at the same time he was a medical worker who got infected. “The curer had to be cured”. “It was weird being a patient brought into the hospital by my co-workers and being treated by people I knew. I used to drive patients and now I was the patient back in the ambulance. You don’t realize how dangerous our work can be unless you become the patient.” He also mentioned that this experience made him realize the fear of the patient, not knowing what will happen.
Asking my parents about the time they received the news about Konstantinos, their reaction, and their feelings, I was finally sure that no matter how prepared you are due to your occupation you never see something like that coming. Theodoros stated that no matter the severity of the situation when a colleague goes down it is a shock for everyone. “When I heard that Konstantinos has contracted the virus and that he was transported to the ICU, I got scared. Firstly because my fellow work-partner was in a critical stage and Dimitra was isolated not being able to contact anyone but also because I saw for the first time what COVID-19 can do to people. Konstantinos literally fought for his life.” My father pointed out that he will never forget the day he saw him at work for the first time, almost 2 months after his recovery. “He was not the Konstantinos I worked with, at least physically. He had lost half his weight, he looked wrecked. But I feel that he was more fearless too. Dimitra was working with us this whole time, after the 15 days of quarantine. It was extremely painful for her and I can only imagine what she has been through. We could not do anything else but support her.” Indeed, a study in the UK has revealed that the pandemic brought medicals teams closer. 10 Alexia also mentioned that hearing the news about Konstantinos and his dire situation, she felt that coronavirus was so dangerous that can send an otherwise totally healthy person to Intensive Care Unit. “One day he was full of energy and life and the other day he was transported to the ICU.”
Knowing that asking such questions may lead my interviewees relive and re-remember those horrible days, I tried to avoid getting into further details. But they granted me the right to ask my parents, close friends of them, for more details about those. So I will collocate what Theodoros and Alexia know about those days. During that period, they kept their life going, applying of course the public health measures. They felt that quarantine brought Dimitra close to depression and anxiety. She has lost interest in everything my parents said. She communicated with Konstantinos only a few times per day and that was not enough. Imagine having your partner in hospital in a very crucial stage and not being able to be there. It was a psychological torture for her. But also for him. He could only know that she was physically healthy, but he was no first-hand knowledge of her emotional condition. He knew that Dimitra suffered, but he could not do anything. My parents both agreed on that “This experience tore them apart but it glued them back together, all their pieces are connected tighter now. They survived so they try to cherish it. It will be a black page in their book but it will be forgotten while the time goes by.”
CONCLUSIONS
We definitely owe a huge thank you to the front-line health workers for being there, for being supporters, caretakers, for just being strong when we cannot. In COVID-19 times, the phrase “heal the healer” conquered the world. 11 In several studies, scholars highlighted vivid physical effects from constantly “fighting against this disease”. They mentioned fatigue, dizziness, anxiety, post-traumatic stress and a clinician burn-out from working extra shifts. 12 It is striking that none of my sources mentioned any of the above. So we could only assume that, may be due to their work-position, they did not experience such a psychological strain. They are all paramedics; they were not so much burdened with treating and saving the COVID-positive patients. But emotionally it is a fact that they were distressed. They were not fearless, because their families could be endangered if they were not careful enough. Something that comes as a closure from the interviews is that their friends and families were their strength and their weakness at the same time. When they come home, they are relaxed and their mind “sails away” from the disease, but when they were at work all they could think of (at least at the beginning) was if they will contract the virus and infect their families. And the pandemic did not only alter the nature of their occupation but also them as personalities. They were in the eye of the cyclone. Their friends and their families got infected but they had to keep doing what they are supposed to, take care of people. Maybe they were not afflicted so much because, despite the high mortality rates, there were not many victims in their town; maybe if they worked in a big city where hundreds of people died every day, they would me be more traumatized. But unlike the majority of other medical related work-positions, during the same period they kept working with patients that had nothing to do with the Coronavirus. Accidents kept happening; people kept getting sick from other viruses. On the other side of the spectrum, nurses have been mostly dealing with COVID-19 patients, even until now. But –and this can serve as an overarching conclusion- contrary to findings of other related studies, routinization can best describe the current emotional status of the Paramedical Staff interviewed for this paper. Being at the center of the virus outbreak for almost a year, the experience gradually became a routine for them. This global crisis altered us and made us revision the future. Responsibility and consciousness are two assets that this pandemic pointed as the cornerstone of our society.
BIBLIOGRAPHY
- “Γιατί η ΜΕΘ Αγρινίου έγινε το πιο επικίνδυνο μέρος της Ελλάδας” (report)
- Aughterson et al., “Psychosocial impact on frontline health and social care professionals in the UK during the COVID-19 pandemic: a qualitative interview study”, British Medical Journal Open 11, 2021
- Canadian Psychological Association, “‘Psychology Works’ Fact Sheet: Emotional and Psychological challenges Faced by Frontline Health Care Providers During the COVID-19 Pandemic”
- Giannis et al., “Impact of coronavirus disease 2019 on healthworkers: beyond the risk of exposure”, Postgraduate Medical Journal 97, 2021
- Que et al., “Psychological impact of the COVID-19 pandemic on healthcare workers: across-sectional study in China”, Journal of General Psychiatry 33.3, 2020
- Vizheh et al., “The mental health of healthcare workers in the COVID-19 pandemic: A systematic review”, Journal of Diabetes and Metabolic Disorders 19.2, 2020
- Α. Η. Wong et al., “Healing the Healer: Protecting Emergency Health Care Workers’ Mental Health During COVID-19”, Annals of Emergency Medicine 4, 2020
INTERVIEWS
- THEODOROS BAKASINIS, 05/05/2021, AITOLOAKARNANIA
- ALEXIA KATSAKIORI , 05/05/2021, AITOLOAKARNANIA
- ANONYMOUS, Interview by the author, 29/04/2021
- ANONYMOUS, Interview by the author, 29/04/2021
NOTES:
*Two of my narrators requested to stay anonymous through the paper. The names “Dimitra” and “Konstantinos” are false names.
- Α. Η. Wong et al., “Healing the Healer: Protecting Emergency Health Care Workers’ Mental Health During COVID-19”, Annals of Emergency Medicine 76.4 (2020): 379-384. ↩
- Α. Η. Wong et al., “Healing the Healer: Protecting Emergency Health Care Workers’ Mental Health During COVID-19”, Annals of Emergency Medicine 76.4 (2020): 379-384. ↩
- M. Vizheh et al., “The mental health of healthcare workers in the COVID-19 pandemic: A systematic review”, Journal of Diabetes and Metabolic Disorders 19.2 (2020):8. ↩
- The adjacent graph is based on monthly statistics about Coronavirus-positive patients. See also the official data at: https://www.in.gr/tags/%CE%BA%CE%BF%CF%81%CE%BF%CE%BD%CE%B1%CF%8A%CF%8C%CF%82/ Last accessed in July 28th, 2021. ↩
- J. Que et al., “Psychological impact of the COVID-19 pandemic on healthcare workers: across-sectional study in China”, Journal of General Psychiatry 33.3 (2020): 8. ↩
- An investigative report, published in mid-June 2021, dubbed the Intensive Care Unit of my hometown as “the most dangerous place in Greece”. See “Γιατί η ΜΕΘ Αγρινίου έγινε το πιο επικίνδυνο μέρος της Ελλάδας”. ↩
- D. Giannis et al., “Impact of coronavirus disease 2019 on healthworkers: beyond the risk of exposure”, Postgraduate Medical Journal 97 (2021): 326-328. ↩
- Α. Η. Wong et al., “Healing the Healer: Protecting Emergency Health Care Workers’ Mental Health During COVID-19”, Annals of Emergency Medicine 76.4 (2020): 379-384. ↩
- Canadian Psychological Association, “Psychology Works” Fact Sheet: Emotional and Psychological challenges Faced by Frontline Health Care Providers During the COVID-19 Pandemic, p.4. ↩
- H. Aughterson et al., “Psychosocial impact on frontline health and social care professionals in the UK during the COVID-19 pandemic: a qualitative interview study”, British Medical Journal Open 11 (2021): p.9. ↩
- Α. Η. Wong et al., “Healing the Healer: Protecting Emergency Health Care Workers’ Mental Health During COVID-19”, Annals of Emergency Medicine 76.4 (2020): 379-384. ↩
- H. Aughterson et al., “Psychosocial impact on frontline health and social care professionals in the UK during the COVID-19 pandemic: a qualitative interview study”, British Medical Journal Open 11 (2021): p.5. ↩